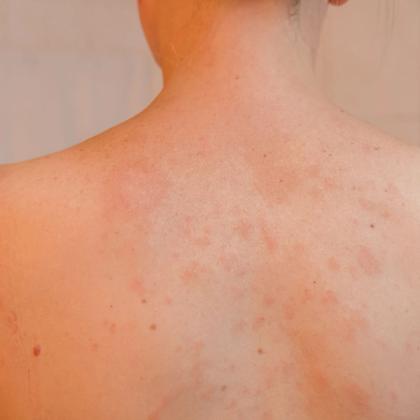
Pityriasis rosea is a common and self-limiting condition, but it can cause significant anxiety and distress for patients. In this episode, Dr Kate Chesterman discusses the expected course and clinical findings that are associated with this condition, as well as exploring possible differentials, treatment options, potential complications and referral criteria.
Key take-home points
- Pityriasis rosea is a common, self-limiting skin condition characterised by pink-red patches and fine, flaky scales.
- Most frequently affects children and young adults (ages 10–35).
- It is not contagious.
- The exact cause is unknown; the strongest evidence links to herpes viruses 6 and 7, possibly due to viral reactivation.
- Drug-induced cases can mimic idiopathic pityriasis rosea and are worth considering, especially in elderly or atypical cases.
- Triggering medications include – among others – angiotensin-converting enzyme inhibitors, antibiotics, biologics, non-steroidal anti-inflammatory drugs and some vaccines.
- Two-thirds of patients experience a prodromal illness (headache, fever, tiredness, sore throat, lymphadenopathy).
- A herald patch (salmon-pink to bright red, 2–5 cm, with a collarette of scale) appears first, usually on the trunk, thigh, upper arm or neck.
- Within 2 weeks, a widespread rash develops with small oval patches, often following Langer’s lines.
- The patches are often pink in light skin. In skin of colour, patches can appear as grey, brown or black.
- The hands, feet and face are usually spared. Oral lesions may occur.
- The rash usually resolves spontaneously in 6–8 weeks. Pigment changes may persist temporarily but do not scar.
- Consider alternative diagnoses if blisters are present, most lesions are on palms or soles or syphilis is suspected.
- Differential diagnosis includes secondary syphilis, tinea corporis, erythema multiforme, guttate psoriasis, viral exanthems and cutaneous T cell lymphoma.
- Most cases require only supportive care: avoidance of soaps, use of emollients and soap substitutes.
- Itch may be managed with mild/moderate topical steroids and oral antihistamines.
- Dermatology referral advised for atypical, prolonged or severe cases.
Key references
- NHS. 2023. https://www.nhs.uk/conditions/pityriasis-rosea/.
- Primary Care Dermatology Society. 2022. https://www.pcds.org.uk/clinical-guidance/pityriasis-rosea.
- Dermnet NZ. 2021. https://dermnetnz.org/topics/pityriasis-rosea.
- Litchman G, et al. StatPearls [Internet]. 2024. https://www.ncbi.nlm.nih.gov/books/NBK448091/.
- Eisman S, et al. BMJ, 2015;351:h5233. doi: 10.1136/bmj.h5233.
- Mashoudy K, et al. Am J Clin Dermatol. 2025;26(2):237-250. doi: 10.1007/s40257-024-00915-7.
- Primary Care Dermatology Society. 2025. https://www.pcds.org.uk/patient-info-leaflets/pityriasis-rosea.
- British Association of Dermatologists. 2023. https://www.bad.org.uk/pils/pityriasis-rosea.
Create an account to add page annotations
Add information to this page that would be handy to have on hand during a consultation, such as a web address or phone number. This information will always be displayed when you visit this page