Antibiotics in acute cough
Choice of antibiotic
Antibiotics in the presentation of cough are only indicated in specific scenarios (1,2):
Acute cough - decision schemata (1):
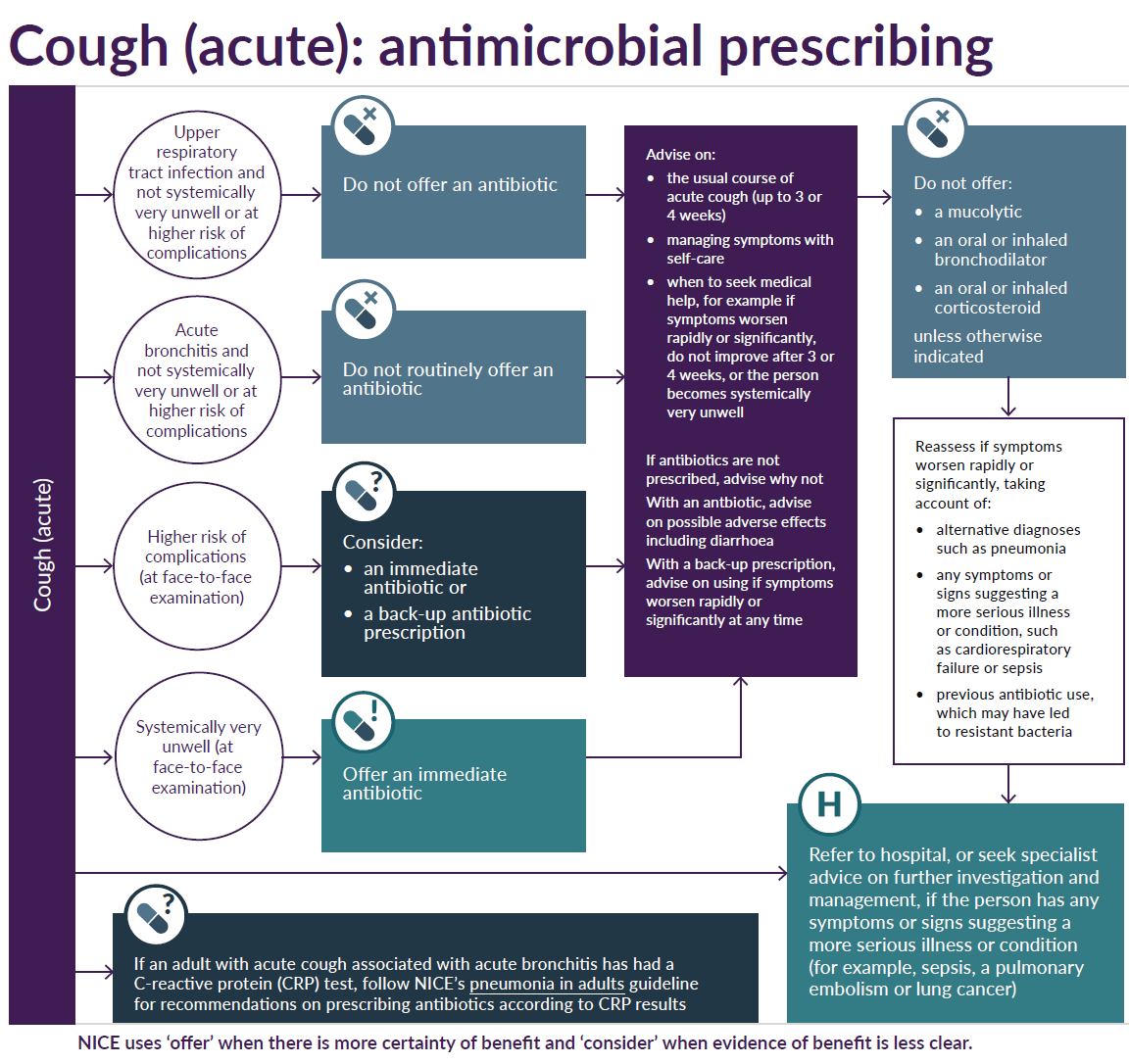
Antibiotics for adults aged 18 years and over (2,7)
First choice:
- doxycycline - 200 mg on the first day, then 100 mg once a day for 4 days (5-day course in total)
Alternative first choices:
- Amoxicillin 500 mg three times a day for 5 days OR
- Clarithromycin 250 mg to 500 mg twice a day for 5 days OR
- Erythromycin 250 mg to 500 mg four times a day or 500 mg to 1,000 mg twice a day for 5 days
Notes:
- See BNF for appropriate use and dosing in specific populations, for example, hepatic impairment, renal impairment, pregnancy and breast-feeding.
- Doses given are by mouth using immediate-release medicines, unless otherwise stated.
- Doxycycline should not be given to pregnant women, and the possibility of pregnancy should be considered in women of childbearing age (BNF, December 2018)
- Amoxicillin or erythromycin are preferred in women who are pregnant.
Antibiotics for children and young people under 18 years
First choice:
- Amoxicillin
- 1 to 11 months, 125 mg three times a day for 5 days
- 1 to 4 years, 250 mg three times a day for 5 days
- 5 to 17 years, 500 mg three times a day for 5 days
Alternative First Choice antibiotics:
- Clarithromycin
- 1 month to 11 years:
- Under 8 kg, 7.5 mg/kg twice a day for 5 days
- 8 to 11 kg, 62.5 mg twice a day for 5 days
- 12 to 19 kg, 125 mg twice a day for 5 days
- 20 to 29 kg, 187.5 mg twice a day for 5 days
- 30 to 40 kg, 250 mg twice a day for 5 days
- 12 to 17 years, 250 mg to 500 mg twice a day for 5 days
- 1 month to 11 years:
- OR
- Erythromycin
- 1 month to 1 year, 125 mg four times a day or 250 mg twice a day for 5 days
- 2 to 7 years, 250 mg four times a day or 500 mg twice a day for 5 days
- 8 to 17 years, 250 mg to 500 mg four times a day or 500 mg to 1,000 mg twice a day for 5 days
- Erythromycin
- OR
- Doxycycline 12 to 17 years, 200 mg on the first day, then 100 mg once a day for 4 days (5-day course in total) Notes:
- See BNF for children for appropriate use and dosing in specific populations, for example, hepatic impairment and renal impairment.
- The age bands apply to children of average size and, in practice, the prescriber will use the age bands in conjunction with other factors such as the severity of the condition and the child's size in relation to the average size of children of the same age. Doses given are by mouth using immediate-release medicines, unless otherwise stated.
- Amoxicillin or erythromycin are preferred in young women who are pregnant
- Doxycycline should not be given to young women who are pregnant, and the possibility of pregnancy should be considered in young women of childbearing age (BNF for children, December 2018)
- Doxycycline 12 to 17 years, 200 mg on the first day, then 100 mg once a day for 4 days (5-day course in total) Notes:
General Points regarding managing cough (1,2,3,4,5,6):
- the need for urgent medical admission (in an adult) can be based on the assessment of factors including:
- respiratory rate - more than 30 breaths per minute
- blood pressure - systolic pressure <90 mmHg, or diastolic pressure <60 mmHg
- pulse - more than 130 beats per minute
- temperature
- altered level of consciousness (1,5)
- oxygen saturation level - < 92%, or central cyanosis
- peak expiratory flow rate - < 33% of predicted (6)
- patients at higher risk of complications - these are defined as:
- if they:
- have a pre-existing comorbidity, such as significant heart, lung, renal, liver or neuromuscular disease, immunosuppression or cystic fibrosis
- are young children who were born prematurely
- are older than 65 years with 2 or more of the following criteria, or older than 80 years with 1 or more of the following criteria:
- hospitalisation in the previous year
- type 1 or type 2 diabetes
- history of congestive heart failure
- current use of oral corticosteroids
- if they:
- when an immediate antibiotic prescription is given, give advice about possible adverse effects of the antibiotic, particularly diarrhoea and nausea
- when a back-up antibiotic prescription is given, give advice about:
- an antibiotic not being needed immediately
- using the back-up prescription if symptoms worsen rapidly or significantly at any time
- Acute cough associated with an upper respiratory tract infection
- do not offer an antibiotic to treat an acute cough associated with an upper respiratory tract infection in people who are not systemically very unwell or at higher risk of complications
- do not offer an antibiotic to treat an acute cough associated with an upper respiratory tract infection in people who are not systemically very unwell or at higher risk of complications
- limited evidence suggests that antihistamines, decongestants and codeine-containing cough medicines do not help cough symptoms
Reference
- Dicpinigaitis PV et al. Acute cough: a diagnostic and therapeutic challenge. Cough. 2009;5:11
- NICE (February 2019). Cough (acute): antimicrobial prescribing
- NICE (December 2014).Pneumonia- Diagnosis and management of community- and hospital-acquired pneumonia in adults
- 2015 - Annotated BTS Guideline for the management of CAP in adults (2009)
- Subbe CP. Validation of a modified Early Warning Score in medical admissions. QJM. 2001;94(10):521-6
- Scottish Intercollegiate Guidelines Network and British Thoracic Society 2009. British guideline on the management of asthma: a national clinical guideline
- Public Health England (June 2021). Managing common infections: guidance for primary care
Related pages
Create an account to add page annotations
Annotations allow you to add information to this page that would be handy to have on hand during a consultation. E.g. a website or number. This information will always show when you visit this page.