Intrauterine insemination (IUI)
Intrauterine insemination (IUI) is an assisted conception technique that involves the deposition of a processed semen sample in the upper uterine cavity, overcoming natural barriers to sperm ascent in the female reproductive tract
- a cost-effective, noninvasive first-line therapy for selected patients with functionally normal tubes, and infertility due to a cervical factor, anovulation, moderate male factor, unexplained factors, immunological factor, and ejaculatory disorders with clinical pregnancy rates per cycle ranging from 10 to 20%
- has limited use in patients with endometriosis, severe male factor infertility, tubal factor infertility, and advanced maternal age >= 35 years (1)
- IUI may be performed with or without ovarian stimulation
- controlled ovarian stimulation, particularly with low-dose gonadotropins, with IUI offers significant benefit in terms of pregnancy outcomes compared with natural cycle or timed intercourse, while reducing associated COH complications such as multiple pregnancies and ovarian hyperstimulation syndrome
- a systematic review found gonadotropins improve cumulative live birth rate vs anti-oestrogens and aromatase inhibitors (2)
- there is no convincing evidence aromatase inhibitors are superior to anti-oestrogens
- none of the agents increased the multiple pregnancy rate
- a systematic review found gonadotropins improve cumulative live birth rate vs anti-oestrogens and aromatase inhibitors (2)
- controlled ovarian stimulation, particularly with low-dose gonadotropins, with IUI offers significant benefit in terms of pregnancy outcomes compared with natural cycle or timed intercourse, while reducing associated COH complications such as multiple pregnancies and ovarian hyperstimulation syndrome
NICE state with respect to intrauterine insemination (3)
- for people with unexplained fertility problems who have tried to conceive for 2 years through regular unprotected vaginal sexual intercourse, discuss the treatment options, including the benefits, risks and their individual preferences and:
- before in vitro fertilisation (IVF) treatment, consider up to 4 cycles of intrauterine insemination (IUI) with ovarian stimulation using gonadotrophins, or
- offer IVF treatment
- if the woman, trans man or non-binary person with endometriosis has not conceived during 2 years of expectant management or after surgical treatment, or if expectant management or surgical treatment (or both) is not appropriate, discuss the fertility treatment options and:
- consider up to 4 cycles of intrauterine insemination (IUI) with ovarian stimulation using gonadotrophins before offering IVF treatment, if appropriate, or
- offer IVF treatment
- for people who are using artificial insemination to conceive and who are concerned about their fertility that:
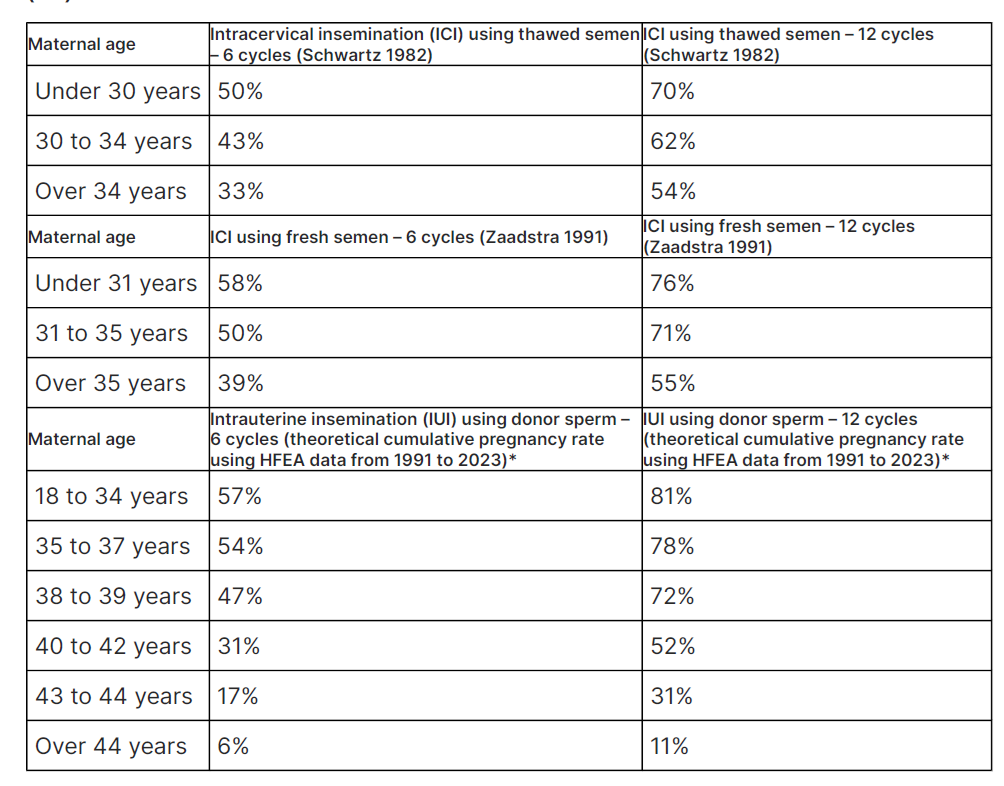
- 47% to 57% (depending on age) of women aged under 40 years will conceive within 6 cycles of intrauterine insemination (IUI)
- of those who do not conceive within 6 cycles of IUI, about half will do so with a further 6 cycles (cumulative pregnancy rate of 72% to 81%, depending on age)
- 12 cycles of unstimulated IUI (providing there are no contraindications) should be offered before considering in vitro fertilisation (IVF) for:
- people who are unable to, or would find it very difficult to, have vaginal intercourse because of a clinically diagnosed physical disability or psychosexual problem
- couples where the partner with male reproductive organs has azoospermia and surgical sperm retrieval is not suitable or has been unsuccessful, and they wish to use donor sperm treatment
- for women, and trans men and non-binary people with female reproductive organs who are using donor insemination and have not conceived after 6 cycles, offer 6 cycles of unstimulated donor IUI (providing there are no contraindications and no suspected or known clinical causes of infertility) before considering IVF
Cumulative probability of conceiving a clinical pregnancy by the number of cycles of insemination – intracervical insemination (ICI) and intrauterine insemination (IUI)
Notes (1):
- transcriptome of spermatozoa used in homologous IUI reveals profound differences between expression profiles of sperm samples that impregnate successfully and those that do not
- these differences might improve the predictive power of sperm evaluation to estimate IUI success by complementing the basic sperm analysis
Reference:
- Allahbadia GN. Intrauterine Insemination: Fundamentals Revisited. J Obstet Gynaecol India. 2017;67(6):385-392. doi:10.1007/s13224-017-1060-x
- Cantineau AEP, Rutten AGH, Cohlen BJ. Agents for ovarian stimulation for intrauterine insemination (IUI) in ovulatory women with infertility. Cochrane Database of Systematic Reviews 2021, Issue 11. Art. No.: CD005356
- NICE. Fertility problems: assessment and treatment. Clinical guideline CG156. Published February 2013, last updated March 2026
Related pages
Create an account to add page annotations
Annotations allow you to add information to this page that would be handy to have on hand during a consultation. E.g. a website or number. This information will always show when you visit this page.